Early diagnosis of cancer improves outcomes by starting treatment at the earliest possible stage when treatment is most likely to be successful. An important step in early diagnosis is spotting changes in your body and bringing them to the attention of your doctor so the reason for the changes can be identified. Self-exams play an important role in helping you spot changes. A good place to start is with your skin.
Skin self-exam
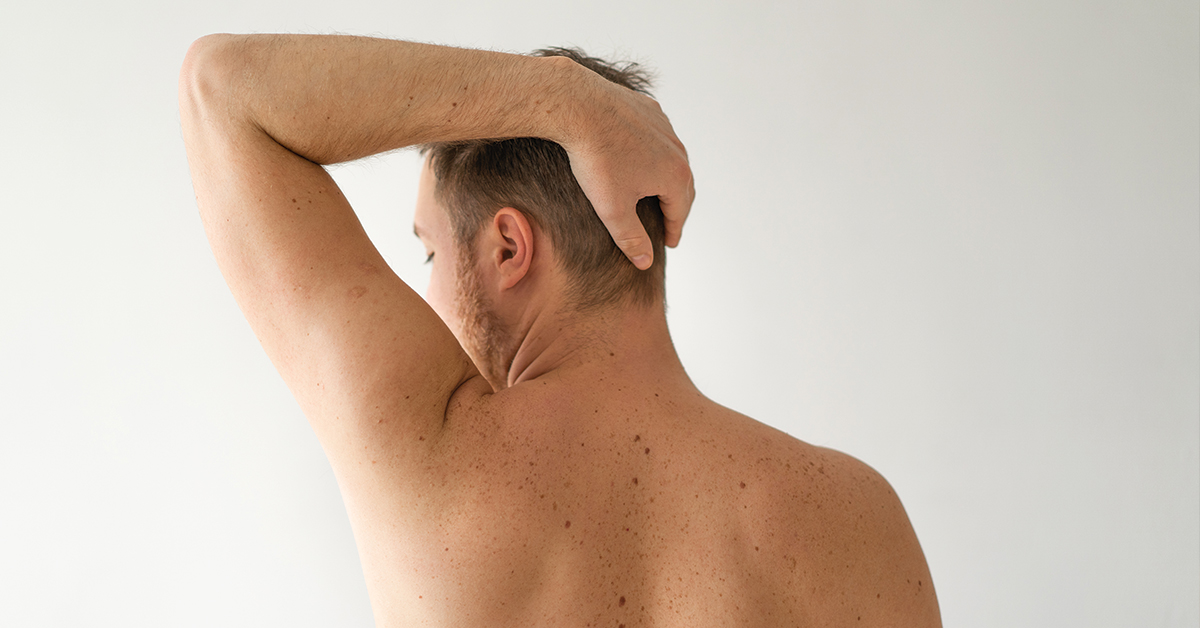
When caught early, skin cancer is highly curable. The best way to recognize changes to your skin is to examine yourself head-to-toe every month.
What to look for:
• A new growth or an existing growth that changes in size and appears pearly, transparent, tan, brown, black, or multicoloured
• A mole, birthmark, or brown spot that gets larger than a pencil eraser, becomes thicker, or changes in texture or colour
• A spot or sore that continues to itch, hurt, bleed, crust, or scab
• An open sore that does not heal within three weeks

How perform a skin self-exam:
• Inspect your face, especially your nose, mouth, and the front and back of your ears. Use mirrors to get a clear view.
• Thoroughly inspect your scalp. Use a blow dryer to separate your hair and expose every section of your scalp so you can view it with a mirror. It may be easier if you can get a family member or friend to help.
• Scan your hands and arms. Look at your palms, the back of your hands, and between your fingers. Continue up your wrists and arms, and don’t forget your underarms.
• Check your torso. Start with your neck and move down to your chest, including the undersides of your breasts, then your abdomen.
• Inspect your back. Stand with your back to a full-length mirror and hold a hand mirror, moving it as needed so you can view your whole back, including your neck, shoulders, upper back, lower back, and buttocks.
• Examine your genitals using a hand mirror.
• Scan your legs, front and back, using a hand mirror where necessary. Start at your thighs, move down your shins to your ankles, and finish with your feet, including the soles and your toes.
Breast self-exam
There is some debate about the value of breast self-exams in detecting breast cancer early when treatment has the best chance of being successful. While some healthcare professionals question the value of these exams, many physicians and health-related organizations firmly believe that breast self-exams are an important screening tool, especially when used in combination with regular physical exams by a doctor, mammograms, and sometimes ultrasound or an MRI.
What to look for:
• A change in size, colour, or shape of the breast
• Any lump, swelling, or distortion
• Breasts that are unevenly shaped
• Dimpling, puckering, or bulging skin
• Redness, soreness, or rash
• A nipple that has changed position or turned inward instead of sticking out
• Signs of fluid coming out of one or both nipples
How to perform a breast self-exam:
• Begin by standing in front of a mirror with your shoulders straight and your hands on your hips, and inspect your breasts carefully, turning from side to side so you can see all areas of your breasts. Alternatively, you can perform the exam while lying down using a hand mirror. If you do it lying down, your breast tissue will spread out and become thinner, making it easier to feel what’s below the skin. Another option is to do it in the shower with your breasts lathered, making it easier for your fingers to glide smoothly across your skin.
• Using the pads of your fingers, not your finger tips, examine your left breast with your right hand and your right breast with your left hand. Keeping your fingers flat and together, use a circular motion to feel for anything unusual. Cover the whole breast area from your collarbone to the top of your abdomen and from your armpit to your cleavage.
Testicular self-exam
A testicular self-exam is a simple pain-free test that helps a male become familiar with his testicles so he will be able to notice any changes.
What to look for:
• A lump
• Pain or swelling in the scrotum
• Any change in size, shape, tenderness, or sensation
• A soft collection of thin tubes above the testicles
• A testicle that you cannot feel because it has not properly descended into the scrotum
How to perform a testicular self-exam:
• This test is best performed standing, either during or just after a shower when the scrotal skin is warm and relaxed.
• Gently feel the scrotal sac to locate the testicles.
• Using one hand to stabilize the testicle, use the fingers and thumb of the other hand to firmly but gently feel the entire surface of the testicle.
• Repeat the procedure on the other testicle.
The next step
Self-exams are just the first step in the early diagnosis of any health problem. If you notice anything unusual or anything that concerns you, see your doctor for further testing to identify the cause of the issue. That way, if there is a problem, it can be addressed at a stage when treatment is most likely to be successful.