Looking forward to warm weather and longer days? Or are you dreading those seasonal allergies? Take charge this season and arm yourself with an allergy toolkit stocked with quality allergy medicine from London Drugs. Prepare ahead of time, find relief when you need it, and enjoy spring and summer to their fullest—sniffle-free.
How to Prepare for Allergy Season
Getting a head start provides longer periods of relief—or even no symptoms at all—rather than the “two steps forward, one step back” cycle that allergy season often feels like. Here are a few ways to prepare for allergy season before it hits.
Know Your Triggers
Understanding whether it’s pollen, dust, pet dander, or snow mould that sets off your allergies keeps you prepared on when to start allergy medications, which types are most effective, and how to reduce these triggers in your home environment.
Start Treatment Early
Allergies can build over time, making symptoms harder to manage. Starting antihistamines like Allegra and Reactine early can prevent reactions such as sneezing, congestion, itchy eyes, or fatigue from fully developing. Start taking them one to two weeks before your region’s allergy season and use them consistently to keep symptoms milder, shorter, and easier to control.
Stock Up On Essentials
The last thing you feel like doing when battling allergies is a quick run to the store, so keep the best tools for you and your family on hand. Antihistamines, tissue, nasal rinses, and children’s allergy formulations should all be in your allergy medicine cabinet.
Check Your Home Environment
Routine checks and cleaning should happen more frequently in an allergy-sensitive home. Wash bedding weekly and change furnace filters monthly. Monitor high-pollen days in your weather app and keep windows closed during peak times.
Plan for Outdoor Exposure
Consider rescheduling outdoor activities when pollen levels are high and begin taking antihistamines the day before. Afterwards, shower if you can, or at the very least, change your clothes to prevent allergens from remaining in contact with your skin for too long.
When to Start Allergy Medications
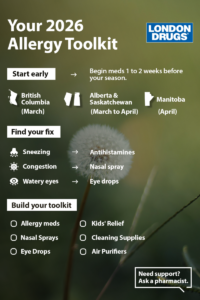
Knowing when to start allergy meds can make a huge difference in how much relief you get from your triggers—waiting until they’re in full swing greatly reduces the effectiveness of your medications. Pharmacists suggest getting ahead of the game by starting your antihistamines 1 to 2 weeks before the season begins. It’s better to be overprepared than to play catch-up with your allergies mid-season.
When Does Allergy Season Start?
Allergy season doesn’t start at the same time across Canada. Here’s a quick breakdown to help you identify when to expect allergies in your region.
- British Columbia: Early March, with tree pollen appearing first
- Alberta and Saskatchewan: Late March to April, depending on snow melt
- Manitoba: April, as temperatures rise and snow mould clears
- Ontario and Quebec: April to May, with tree pollen followed by grass
- Atlantic Canada: Late April to May, with a slightly delayed start due to the coastal climate
Take Snow Mould Allergies Into Account
As snow melts, snow mould spores can trigger early allergy symptoms, especially in the Prairies, Ontario, and Quebec. If snow mould allergies affect you, start your allergy routine early and avoid damp outdoor areas to reduce exposure and prevent early-season flare-ups.
LD Tip: Talk to a Pharmacist for Guidance
Pharmacists at London Drugs are available for guidance on minor ailments and over-the-counter treatments. They can also help you approach your allergies holistically by assessing your symptoms, identifying patterns of when they improve or worsen, and offering lifestyle recommendations that you may not have considered.
Build Your Allergy Toolkit Before Symptoms Peak
Preparedness is prevention, especially when it comes to seasonal allergies. Make sure your home is stocked with essentials from each of these categories, and you’ll be ready for whatever comes your way this season.
Allergy Medications
Oral antihistamines are a must-have. Products like Allegra and Aerius are designed for daily use to keep symptoms under control and interrupt the allergy response cycle. Others, like Benadryl and Reactine, can be used as boosters for breakthrough symptoms and provide fast-acting relief at the onset of irritation. Shop allergy medications at London Drugs for the best allergy products in Canada.
Children’s Allergy Relief
While adult and children’s allergy medications can contain the same active ingredients, it’s important not to guess on the correct dose and delivery system. Keep children’s allergy relief on hand, and make a note of the differences between infant and general children’s formulations. Talk to a pharmacist if you’re unsure which allergy meds are best for your child.
Eye Drops
Eye drops for allergies from brands like Bausch & Lomb can help relieve dryness and flush out irritants, while antihistamine drops from brands like Alcon can target itchiness and redness for fast relief.
Nasal Sprays and Rinses
Sinus products, such as nasal sprays and rinses, are formulated to help with allergy-related stuffiness and dryness. Nasal sprays can provide highly effective relief from congestion, but read the manufacturer’s instructions and use them carefully. Overuse can lead to rebound congestion, causing prolonged stuffiness even after any irritants subside. Nasal rinses, on the other hand, are safe to use as needed and can prevent additional irritations caused by repeated nose-blowing. Ask a pharmacist for help deciding which type is best for your needs.
Air & Home
Air purifiers are among the most effective tools for controlling indoor allergens. Place them in common areas and bedrooms, leaving enough space around them to allow proper air circulation. Brands like Honeywell and Winix last for years with regular filter changes, helping keep your home environment a safe zone for you and your family.
Cleaning Supplies
The last line of defense against allergens in your home is maintaining a clean environment. Stock up on cleaning essentials, such as gentle, low-irritant products, and supplies to remove dust and allergens from carpets and surfaces.
LD Tip: Skip the Line with Delivery & Pickup Options
London Drugs is your one-stop shop for everything from OTC allergy medications to creating an irritant-free home for you and your family. From daily antihistamines and nasal care to air purifiers and cleaning supplies, London Drugs has everything you need to support allergy relief. Shop online for home delivery or find a store near you for easy in-store pickup.
How Pharmacists Can Support You Throughout the Season
If you’re not getting the results you want, your local London Drugs pharmacist can help you take a more personalized approach. They provide consultations for minor ailments and, where appropriate, help identify patterns in your symptoms. LD pharmacists are trained to recommend both medication and holistic strategies, and they can help guide you on environmental changes at home and in your daily routine. Talk to a pharmacist today for personalized support in managing your allergy symptoms.
Shop Allergy Essentials at London Drugs
Allergy season doesn’t have to mean months of discomfort. With early preparation, the right toolkit, and support from knowledgeable pharmacists, it’s easy to reduce symptoms and enjoy the season. Shop allergy essentials at London Drugs to stock up on supplies. For additional advice, talk to a pharmacist about managing your allergy symptoms.