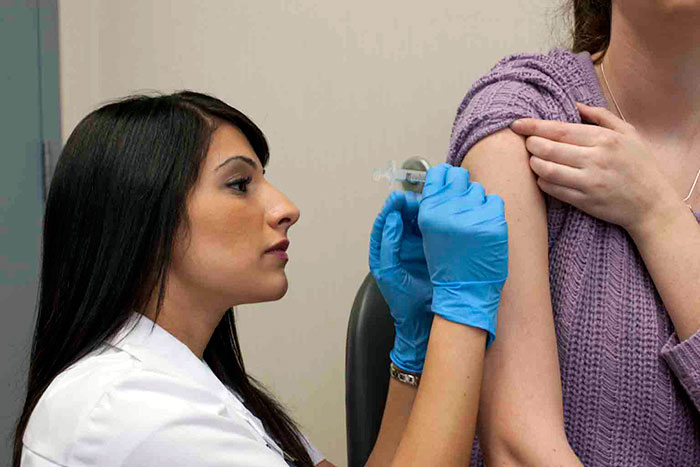
Right about now, all across Canada, many families are in a quandary. The concern for some people, particularly those with school-age children, is whether or not to have a flu shot. While health authorities advise that having the influenza vaccine is the best way to avoid a bout with the flu—and possibly passing it on to others—alternative health proponents and magazines suggest otherwise, often saying it is “safer” to rely on botanical preparations, homeopathic immunity shots and healthy eating.
Right about now, all across Canada, many families are in a quandary. The concern for some people, particularly those with school-age children, is whether or not to have a flu shot. While health authorities advise that having the influenza vaccine is the best way to avoid a bout with the flu—and possibly passing it on to others—alternative health proponents and magazines suggest otherwise, often saying it is “safer” to rely on botanical preparations, homeopathic immunity shots and healthy eating.
While we agree that healthy living makes a positive contribution to an effective immune response, flu viruses are ubiquitous, opportunistic, and unpredictable. Often, despite taking all the health-enhancing steps to avoid catching the virus, we fall prey to it, simply by being close to someone who coughs or sneezes on us, or touching something like a door handle that is contaminated with it.
For some parents, the decision to give their child/ren a flu shot can be fraught with emotion and feelings of guilt brought on by the reactions of other parents who pursue a more “natural” lifestyle.
Ultimately, the decision to have an influenza vaccination rests with the individual, or parent of a minor, but we’d like to clarify a few misconceptions about the flu shot that often result in someone coming down with the virus because they were under the impression that the vaccine is unsafe.
Persistent myths
Let’s take a look at some of the more persistent beliefs about influenza vaccine and vaccinations.
Flu is not a serious disease. If I catch it, I will soon get over it.
To people who have not had flu, or who have experienced a milder strain of flu, this belief is a justifable reason not to have a flu shot. However, flu strains vary, as do individual immune responses, and some strains can have far worse effects than others. It’s important to recognize that flu is not simply a “bad cold.” Rather, it is a serious viral infection that can make you feel rotten for weeks, and keep you away from work and other activities. Furthermore, many people decide to travel in the winter months, and face greater risk of contracting viral infections in the recirculated air of airplane interiors.
During flu seasons where influenza strains are particularly severe, thousands of Canadians may die from flu or its complications—such as pneumonia. Among seniors and other high risk groups, even milder strains of flu can lead to serious illness. A flu shot, particularly if you associate with people who are at high risk, helps protect those people as well as yourself.
The flu shot gives you flu and should therefore be avoided.
While it is true that influenza vaccine contains flu viruses, these are deactivated (dead)* and are unable to give you flu. Experts believe that two factors are responsible for this persistent belief: First, some people have an achy feeling after receiving the vaccine. This side effect has nothing to do with flu and leaves within a day or so. Second, the start of flu season—and flu shots—coincides with the appearance of many bugs that cause winter ills. Catching one of these is relatively easy, yet people often prefer to blame their recent flu shot.
* The exception is live attenuated nasal influenza vaccine (FluMist ®), which contains live flu virus engineered to inactivate the components of the virus that make people sick. As a precaution, people with compromised immune systems are advised not to have this type of vaccine.
Having a flu shot can result in severe reactions or side effects.
Most people who get the flu shot only experience redness, soreness or minor swelling where the vaccination was given. Some people, particularly when having their frst flu shot, may develop a headache, muscle aches or tiredness.
Vaccines contain dangerous ingredients like thimerosal.
This belief surfaced following media reports linking the preservative thimerosal—which contains ethyl mercury—to autism. However, multiple studies have shown no evidence of a link. Health Canada advises that thimerosal, which is only present in influenza vaccine, contains ethyl mercury in an amount well below established limits of safety. Ethyl mercury is eliminated from the body rapidly and does not accumulate, even in premature infants. (This is in contrast to methyl mercury which is found in many foodstuffs, especially fsh. This form of mercury remains in the body longer and can accumulate.)
I am pregnant, so I shouldn’t get a flu shot.
Influenza vaccine is considered safe at any stage of pregnancy. Since pregnancy can put additional stress on the heart and lungs and can also affect the immune system, having a flu shot can help prevent flu-related complications.There is also some evidence to suggest that flu during pregnancy can increase the risk of miscarriage, premature birth and low birth weight.
A flu shot during pregnancy can also protect your baby following birth, since babies cannot have influenza vaccine until they are 6 months old. When you have a flu shot during pregnancy, the antibodies you develop will pass through the placenta to help protect your baby from the flu. A 2011 study showed that babies whose mothers had a flu shot during pregnancy were nearly 50 per cent less likely to be hospitalized with the flu during their first flu season than babies whose mothers remained unvaccinated.
I wrap up warm and hardly ever go out in the cold so I don’t need vaccine to protect me.
Although we may shiver and shake when it’s cold out, this is simply the body’s attempt to generate heat and stay warm. It has nothing to do with catching a cold or flu virus. It just happens that flu season in North America coincides with the colder weather. In other words, wearing that winter toque and snuggly jacket won’t protect you in the same way as the influenza vaccine will.
We hope these insights will help you reach a decision with respect to influenza vaccinations that will provide you and your loved ones with the best protection possible from the flu this coming season.
better care™ Healthy Lifestyles is published three times a year by London Drugs for people interested in health care information. Please address all correspondence to:
The Editor, bettercare™ Healthy Lifestyles, London Drugs, 12831 Horseshoe Place, Richmond, B.C. V7A 4X5.
Articles are reviewed for accuracy, however, the information and suggestions in this publication are for general information only and are not intended to replace medical advice provided by a certified medical professional. London Drugs and the publisher cannot accept liability for any action or decision taken in reliance of this publication. Please seek the advice of your physician or pharmacist if you have any questions or concerns on medical or pharmaceutical matters.
Please note that the people shown throughout this publication are models. As such, their services are provided for illustrative purposes only and should not imply they suffer from the medical condition described in the associated article. Pharmacy shots portray our own pharmacists.
Benowitz I, Esposito DB, Gracey KD, Shapiro ED, Vázquez M, Influenza vaccine given to pregnant women reduces hospitalization due to influenza in their infants. Oxford Journals Medicine & Health Clinical Infectious Diseases Volume 51, Issue 12 Pp. 1355-1361.

 Because long-term excess sunlight exposure raises the risk of at least two very common eye disorders.
Because long-term excess sunlight exposure raises the risk of at least two very common eye disorders.


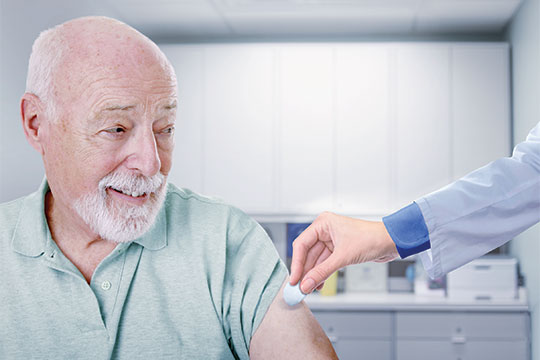

 Right about now, all across Canada, many families are in a quandary. The concern for some people, particularly those with school-age children, is whether or not to have a flu shot. While health authorities advise that having the influenza vaccine is the best way to avoid a bout with the flu—and possibly passing it on to others—alternative health proponents and magazines suggest otherwise, often saying it is “safer” to rely on botanical preparations, homeopathic immunity shots and healthy eating.
Right about now, all across Canada, many families are in a quandary. The concern for some people, particularly those with school-age children, is whether or not to have a flu shot. While health authorities advise that having the influenza vaccine is the best way to avoid a bout with the flu—and possibly passing it on to others—alternative health proponents and magazines suggest otherwise, often saying it is “safer” to rely on botanical preparations, homeopathic immunity shots and healthy eating.